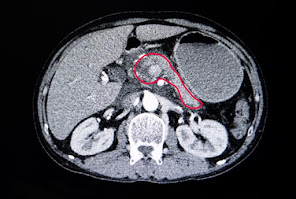
Pancreas is an important endocrine organ which is located behind the stomach. It plays a vital roe in the process of digestion as it produces ‘enzymes’. The enzymes help the body in digestion of fats, proteins and carbohydrates.
What is Pancreatic Cancer?
An abnormal growth of the cells in the pancreas can lead to pancreatic cancer. It occurs within the pancreas tissues and because of this, it can be a little difficult to detect pancreatic cancer. In most cases, the patients do not show any serious symptoms, but just some subtle signs that include:
- Pain in the stomach
- Loss of appetite
- Blood clots
- Unexplained loss in weight
- Depression
- Jaundice
What are the Causes of Pancreatic Cancer?
The exact reason that can lead to pancreatic cancer is still unknown, however it has been established that when cells in the pancreas start to grow at an unusual rate, it can lead to cancer of the pancreas.
All cells have a life circle and the grow and expire in proportion, but sometimes over production of cells makes the old and damaged cells take over the healthy ones leading to infections and thus cancer.
What are the Treatments Available for Pancreatic Cancer?
A great deal of the treatment depends on the stage of cancer as well as the condition the patient is in. However, every treatment has two main objectives:
- Getting rid of the cells that are cancerous
- Preventing the spread of this disease
The available options for treatment are:
X-rays and high-energy beams are used to kill the cancerous cells, and stop their spread to the rest of the body.
Using cancer-killing medications the future growth of cells can be contained.
Certain drugs that are specially designed to destroy only the cancer cells, work very well without harming the healthy cells.
Though a surgery is generally taken as the last option, it depends on the stage at which the cancer has reached. With a surgical procedure a part or parts or the whole pancreas may be removed. There are many factors that your doctor and surgeon will bear in mind before advising a surgery.
Is Pancreatic Cancer Curable?
Yes, it is. However, it largely depends on the stage at which the cancer was detected. An early diagnosis can prove very beneficial for the patient, as with time and age cancer becomes very complex to treat and may return even after a surgery.
Mail Us: gastrosurgeonchennai@gmail.com